Overview
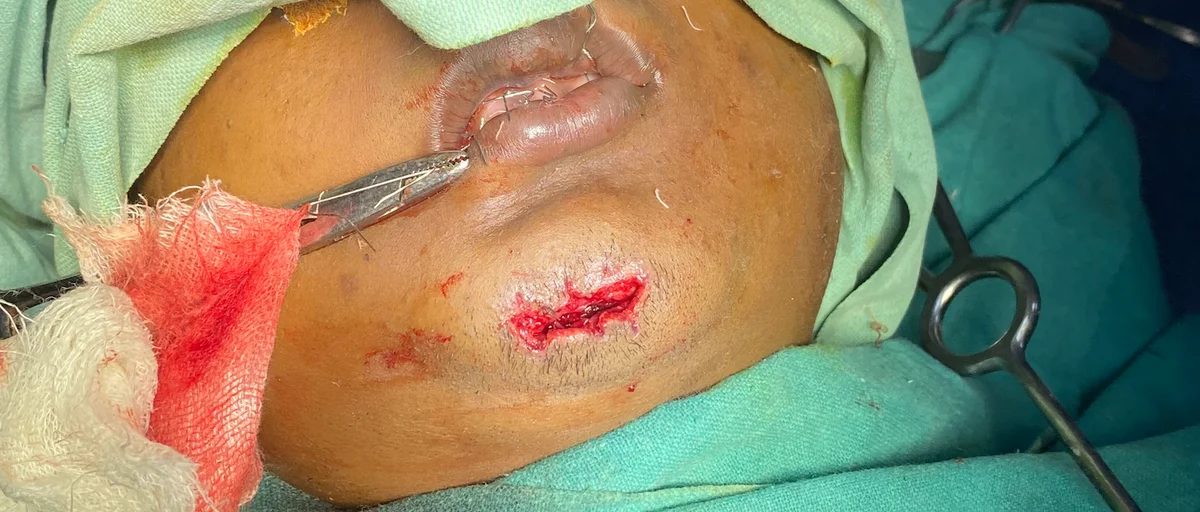
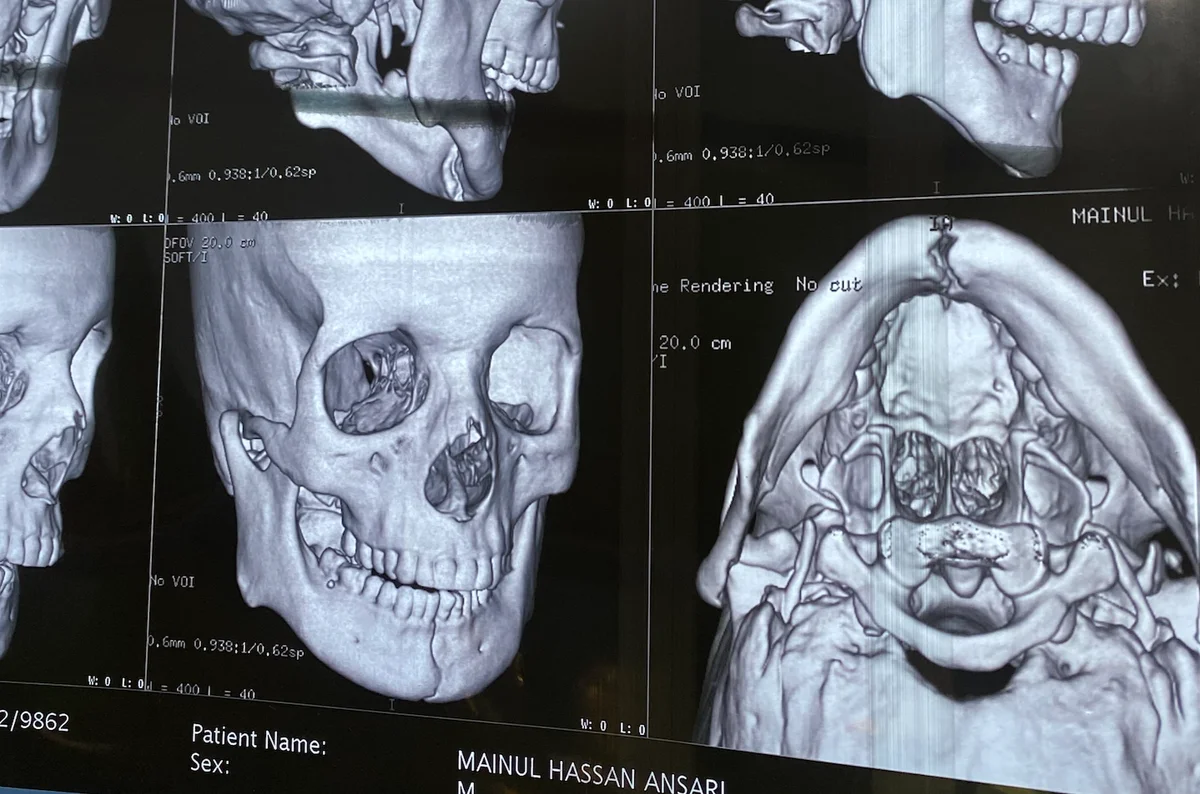
A jaw fracture (mandibular or maxillary fracture) is a break in one or more of the bones of the jaw. The lower jaw (mandible) is the most commonly fractured facial bone, accounting for a significant proportion of all facial fractures seen in emergency departments. The upper jaw (maxilla) may also fracture, often as part of more complex midface injuries.
Jaw fractures occur following road traffic accidents, falls, assaults, sports injuries, or industrial accidents. Because the mandible forms a ring-like structure, forces applied to one part of the jaw frequently cause fractures at two sites simultaneously — for example, a blow to the chin often fractures the symphysis (front of the jaw) and one or both condyles (the jaw joints) at the same time.
Treatment of jaw fractures requires specialist maxillofacial surgical expertise. Dr. Abhisek Chatterjee manages jaw fractures at Asha Nursing Home and Rampurhat Government Medical College, providing emergency and elective surgical care for patients across Birbhum.